After an extensive literature search, this is the first reported case of pilomatrixoma of the breast in Oman. We share this rare case with a brief review of the currently available literature.
Case Report
A 51-year-old man with no comorbidities presented with six months of swelling on his right breast. Though the swelling did not increase in size over time, it was associated with pricking pain. No nipple discharge was noted. There was no history of trauma. Family history revealed that his mother had breast cancer.
On examination, both breasts looked symmetrical with normal nipple-areolar complex. A small nontender, hard 2.0 × 1.0 cm lump was noted at two o’clock in the right breast attached to unremarkable skin. Mammography showed a well-defined dense lesion on the medial aspect of the periareolar region measuring 1.6 × 1.0 cm with peripheral microcalcifications [Figure 1]. Ultrasound of the right breast also confirmed the presence of a well-defined homogeneous, hypoechoic, subcutaneous oval lesion of similar dimensions located 0.5 cm from the nipple [Figure 2]. The lesion was excised under local anesthesia in thebreast clinic.
 Figure 1: Mammography of the right breast showing well-defined isodense opacities with fat content and dense calcifications medially in the periareolar region.
Figure 1: Mammography of the right breast showing well-defined isodense opacities with fat content and dense calcifications medially in the periareolar region.
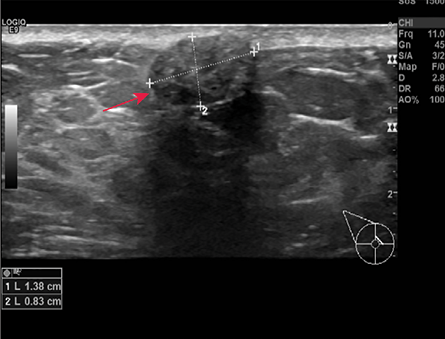 Figure 2: Ultrasound of the right breast showed a well-defined homogeneous, hypoechoic, subcutaneous oval lesion measuring 1.4 × 0.8 cm
Figure 2: Ultrasound of the right breast showed a well-defined homogeneous, hypoechoic, subcutaneous oval lesion measuring 1.4 × 0.8 cm
at three o’clock, 0.5 cm away from the nipple.
The resected specimen was subjected to histopathological examination. Grossly, it was a well-circumscribed, firm, oval nodule measuring 2.0 × 1.7 × 1.7 cm with an overlying ellipse of skin measuring 1.8 × 0.6 cm [Figure 3]. On slicing, the nodule showed a solid, yellow, and gritty cut surface due to areas of calcification. Microscopic examination revealed a neoplasm in the dermis composed of solid nests of basaloid cells undergoing abrupt trichilemmal-type keratinization resulting in eosinophilic ‘shadow’ or ‘ghost cells’ [Figure 4]. Also noted in the stroma were scattered foci of calcification with foreign body reaction and infiltration by chronic inflammatory cells [Figures 5 and 6]. These findings were consistent with pilomatrixoma. When the patient visited the clinic 10 days after the excision, his wound had healed well. He was reassured that the lesion was benign and completely excised.
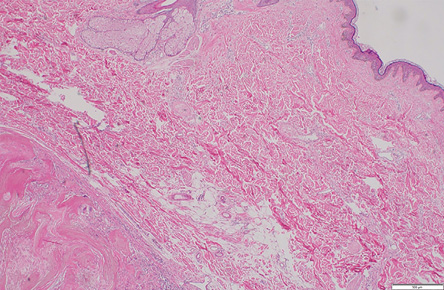 Figure 3: Overlying normal epidermis with a well-circumscribed dermal lesion on the extreme left
Figure 3: Overlying normal epidermis with a well-circumscribed dermal lesion on the extreme left
(hematoxylin and eosin stain, magnification = 50 ×).
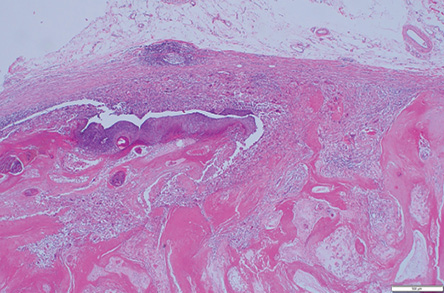 Figure 4: Scanner view of pilomatrixoma comprising all the components viz. basaloid cells, ghost cells, and giant cells (hematoxylin and eosin stain, magnification = 50 ×).
Figure 4: Scanner view of pilomatrixoma comprising all the components viz. basaloid cells, ghost cells, and giant cells (hematoxylin and eosin stain, magnification = 50 ×).
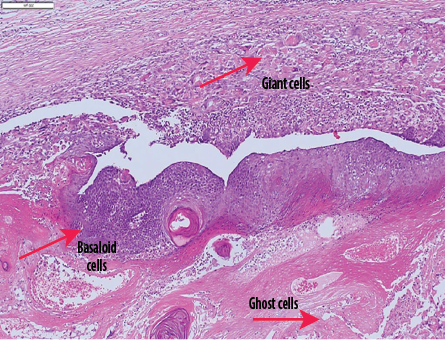 Figure 5: Microphotograph of pilomatrixoma comprising nests of basaloid cells, ghost cells, and multinucleated giant cells (red arrows) (hematoxylin and eosin stain, magnification = 100 ×).
Figure 5: Microphotograph of pilomatrixoma comprising nests of basaloid cells, ghost cells, and multinucleated giant cells (red arrows) (hematoxylin and eosin stain, magnification = 100 ×).
 Figure 6: Ghost cells and multinucleated giant
Figure 6: Ghost cells and multinucleated giant
cells (hematoxylin and eosin stain, magnification
= 200 ×).
Discussion
Pilomatrixoma, also known as pilomatricoma or ‘calcifying epithelioma of Malherbe’ was first recognized in 1880 by Malherbe and Chenanatais.1 It is a rare, slow-growing benign neoplasm originating from the hair matrix, more common in children and young adults with a slight female preponderance.2 While pilomatrixoma can develop in any hair-bearing skin, it is most commonly seen in the head and neck regions. Less commonly, they are noted in the upper extremities, trunk, and lower extremities.3 Pilomatrixoma’s appearance in the breast is considered rare (1:100 000 people). After an extensive literature search, we found nine cases of pilomatrixoma of the breast in adult males reported in the English language [Table 1].
Table 1: Reported cases of pilomatrixoma of the breast in adult males.
|
Hubeny et al.3 2011
|
53
|
Painless, hard, right sided breast lump
|
Mammography: well-circumscribed, oval-shaped mass of the medial right breast, with smooth borders, and multiple small punctuate calcifications.
Ultrasound: small superficial isoechoic well-marginated oval mass parallel to the skin, with smooth borders, and multiple hyperechoic foci.
|
Surgical excision
|
|
Tokur et al.4
2021
|
42
|
Painless, firm, right sided breast mass
|
Mammography: well-circumscribed, approximately 3 × 2 cm, oval density with coarse and fine pleomorphic calcifications in the centrally located lesion in the right breast.
Ultrasound: heterogeneous echo pattern with significant acoustic shadowing due to calcifications in the mass.
|
Surgical excision
|
|
Alsharif et al.5
2015
|
43
|
Painless, firm, left sided breast mass with bluish skin discoloration
|
Mammography: single, superficial, well-defined, and encapsulated 2.3 cm mass containing amorphous microcalcifications in the inferomedial aspect of the left breast.
Ultrasound: well-defined subcutaneous isoechoic mass containing multiple bright foci.
|
Surgical excision with wide margins
|
|
Kapoor et al.6 2018
|
48
|
Painless, firm, left sided breast lump
|
Mammography: solitary oval, well-circumscribed, high-density focal mass in the lower inner quadrant of the left breast with a radiolucent halo.
Ultrasound: well-defined oval, hypoechoic solid mass measuring 1.0 × 3 × 0.8 cm in the periareolar region at the 6–7 o’clock position in the subcutaneous tissues.
|
Surgical excision
|
|
Gil et al.7
2016
|
69
|
Painless, palpable, erythematous, ulcerative left sided breast mass
|
Mammography: irregular, exophytic high-density mass with dystrophic calcifications and coarse heterogeneous calcifications.
Ultrasound: irregular, indistinct, exophytic hyperechoic mass.
|
Surgical excision
|
|
Martins et al.8
2014
|
47
|
Painful, firm, right sided breast nodule
|
Mammography: nodule with indistinct limits and microcalcifications.
Ultrasound: lobulated node, isoechoic, parallel to the skin, with multiple hyperechoic foci.
|
Surgical excision
|
|
Ward et al.9
2019
|
56
|
Painless, firm, left sided breast lump
|
Mammography: circumscribed mass, within superficial subcutaneous fat, abutting the skin undersurface, within the left breast at 9 o’clock,
12 cm from the nipple.
Ultrasound: 1.8 cm oval circumscribed and mildly hypoechoic mass, inseparable from the
skin undersurface.
|
-
|
|
Clark et al.10
2019
|
36
|
Painless hard, left sided breast lump
|
Mammography: oval-shaped, circumscribed mass, in the upper outer left breast, with smooth borders, and multiple pleomorphic calcifications.
Ultrasound: 1.0 × 0.8 × 0.6 cm superficial isoechoic circumscribed oval mass, parallel to the skin and chest wall, with internal vascularity, and multiple hyperechoic foci.
|
Surgical excision was recommended (not done due to financial constraints)
|
These tumors are usually sporadic but around 75% of the cases have mutations in the CTNNB1 gene (which regulates beta-catenin), thereby triggering quick, uncontrolled division of matrix cells leading to pilomatrixoma. Some cases were also found to be related to Gardner syndrome and myotonic dystrophy.12 The exact pathogenesis of pilomatrixoma is still unclear, however, some suggest that recurrent skin trauma induces an inflammatory response leading to hair matrix overgrowth while others consider them to be hamartomas.11 It usually presents as an asymptomatic, single, subcutaneous, firm nodule attached to the skin, sized 1–3 cm. Rarely, they may grow > 5 cm (giant pilomatrixoma). Some of these lesions may be associated with red-blue discoloration of the skin and ulceration.13
Mammography commonly demonstrates a dense mass with multiple, irregular, pleomorphic microcalcifications.10 In addition, Sonography may show a well-circumscribed, oval mass with internal echogenic foci and a peripheral hypoechoic rim, as it did in the present case. If these lesions get calcified, they would appear as hyperechoic masses with posterior acoustic shadowing.
Although imaging studies are useful in determining the size and location of the lesion, core needle biopsy is the modality of choice for confirmation of diagnosis. Histopathological features typically consist of two types of cells surrounded by foreign-body giant cells and calcifications. These are ‘shadow’ or ‘ghost’ cells which are located centrally and basophilic cells at the periphery.10
Pilomatrixomas are benign and the tendency to develop into malignancy is extremely rare with very few reported cases of pilomatrix carcinoma. The majority of the literature agrees on surgical excision as the treatment of choice.9 It serves the cosmetic purpose and prevents the rare possibility of malignant transformation of the tumor. On the other hand, some suggest a conservative approach for patients with a small superficial breast mass showing benign imaging characteristics. These include masses of breast imaging-reporting and data system category 3 without pathologic diagnosis or benign biopsy results.3
Conclusion
Pilomatrixoma in the male breast is a rare benign lesion. It can mimic breast carcinoma because of associated calcification. Therefore, it is prudent to consider pilomatrixoma as a differential diagnosis in patients presenting with superficially located breast lumps.
Disclosure
The authors declared no conflicts of interest. A written consent was obtained from the pateint.
references
- 1. Viero RM, Tani E, Skoog L. Fine needle aspiration (FNA) cytology of pilomatrixoma: report of 14 cases and review of the literature. Cytopathology 1999 Aug;10(4):263-269.
- 2. Imperiale A, Calabrese M, Monetti F, Zandrino F. Calcified pilomatrixoma of the breast: mammographic and sonographic findings. Eur Radiol 2001;11(12):2465-2467.
- 3. Hubeny CM, Sykes JB, O’Connell A, Dogra VS. Pilomatrixoma of the adult male breast: a rare tumor with typical ultrasound features. J Clin Imaging Sci 2011;1:12.
- 4. Tokur O, Aydın S. Seher ztekin P, Süleyman M, Erel S, Celepli P. Pilomatrixoma of the breast in a male patient. Imaging Interv 2021;1:44-146.
- 5. AlSharif S, Meguerditchian A, Omeroglu A, Lamarre P, Altinel G, Mesurolle B. Pilomatricoma of the male breast: sonographic mammographic MRI features with pathologic correlation. Clin Imaging 2015;39(2):308-310.
- 6. Kapoor A, Narayanan R, Tandon A, Santosh AK. Pilomatricoma: an unusual cause of lump in a male breast. J Clin Ultrasound 2018 Mar;46(3):209-211.
- 7. Gil JR, Herh SJ, Kim Y, Song MA, Kim M, Kim EK. A pilomatricoma misdiagnosed as male breast cancer. J Korean Soc Radiol 2016;74(3):156-159.
- 8. Martins MM, Lucarelli AP, Aldrighi JM, Forattini A. A case report of calcifying epithelioma of malherbe (pilomatrixoma) mimicking breast carcinoma in male patient. Case Reports in Clinical Medicine 2014;3:276-280.
- 9. Weng G, Li F, Xu M. Pilomatrix carcinoma of the male breast: a case report. Int J Clin Exp Pathol 2020 Aug;13(8):2153-2157.
- 10. Clark A, Leddy R, Spruill L, Cluver A. Pilomatrixoma, a rare mimicker of male breast cancer. J Clin Imaging Sci 2019 Nov;9:46.
- 11. Sood N, Raj B. Pilomatricoma male breast, mimicking breast carcinoma-a rare case. Indian J Pathol Microbiol 2021;64(1):204-205.
- 12. Ward RC, Donegan L, Khalil H, Wang Y. Pilomatricoma of the male breast. Breast J 2019 Sep;25(5):1012-1013.
- 13. Lin SF, Xu SH, Xie ZL. Calcifying epithelioma of malherbe (Pilomatrixoma): clinical and sonographic features. J Clin Ultrasound 2018 Jan;46(1):3-7.