The Japanese encephalitis virus (JEV) is an important cause of encephalitis in Southeast Asia and the Western Pacific region. Its transmission is primarily by the vector mosquito Culex tritaeniorhynchus through zoonotic cycles, mostly between pigs and wild birds, with humans as incidental dead-end hosts. As the amplifying hosts tend to be most abundant in agricultural areas such as farms and rice paddies where flooding irrigation attracts wading birds, most infections occur in rural areas.1 Although, most infections are asymptomatic, the manifestation of this virus can range from non-specific febrile illness to multiple neurological complications.2
A systematic review of Japanese encephalitis (JE) disease burden estimated that approximately 68 000 JE cases typically occur annually (overall incidence: 1.8 per 100 000), of which only about 10% are reported to the World Health Organization (WHO).3,4 Approximately 33 900 (50%) of these cases occurred in China, and about 51 000 (75%) cases were among children aged 0–14 years (incidence: 5.4 per 100 000). An estimated 55 000 (81%) cases occurred in areas with well-established or developing JE vaccination programs, while 12 900 (19%) cases were from areas with minimal or no JE vaccination programs.5 In a 2015 surveillance, the WHO received reports of 4087 JE cases from 20 (83%) of 24 endemic countries [Figure 1], of which 87% of these cases were reported from four countries: China, India, Nepal, and Vietnam.6 In addition, the Advisory Committee on Immunization Practices (ACIP) reported that among those annual cases, an estimated 20%–30% of patients died, and 30%–50% of survivors had neurologic or psychiatric sequelae.7
The introduction of JE vaccination is therefore important to reduce the disease’s burden, particularly its incidence, as it may cause severe complications such as encephalitis that could lead to permanent neurologic or psychiatric sequelae.4 JE vaccination nationwide since the 1980s has increased the seroprevalence of JEV in some endemic countries, with higher seropositivity seen in adults and the elderly compared to those of younger ages, suggesting natural infection or natural boosting of immunity through exposure to wild virus.8,9 The dynamics of JEV seroprevalence fluctuations indicate that continuous research is important for future prevention and control activities of JEV infection. By stratifying JEV seroprevalence by age, a human population profile of JEV’s immunity and susceptibility can be identified, influencing decision-making on national or subnational vaccination programs. There is a lack of systematic review studies on JE seroepidemiology in recent years. Thus, this study aimed to determine the trend of age-specific JEV seroprevalence in JE endemic countries using results available from studies conducted in the past decade.
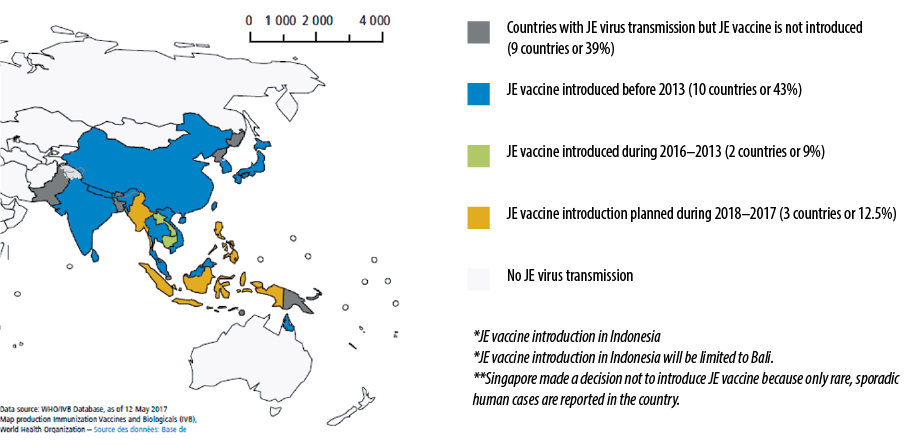
Figure 1: Map of areas with risk of Japanese encephalitis (JE) virus transmission and JE vaccine introduction, 2016.
Methods
A systematic search was conducted between November and December 2019 for all reported studies on JEV seroprevalence published between 2010 and 2019. The literature search was performed in two databases, PubMed and Web of Science, according to the PRISMA guidelines. The keywords used were: ‘Japanese encephalitis’ and ‘Seroprevalence’ or ‘Seropositivity’ or ‘Seroepidemiology’ or ‘Serosurvey’ or ‘Immunity’ or ‘Antibody’.
The target population of this search was subjects who had been investigated for JEV status by serology. The inclusion criteria from the database searches were: (a) quantitative studies that fulfill the keywords and terms searched; (b) availability of full-text articles; (c) original articles; and (d) English-language articles. The exclusion criteria in this search were based on: (a) types of article (case study, review paper, non-peer reviewed articles); (b) clinical JE studies (serostatus of a patient with confirmed JE); (c) vaccine trial studies; and (d) non-human seroprevalence studies (pigs, horses, birds, chickens, or mosquitoes). Articles were then identified through titles and abstracts were screened using the eligibility criteria. The flow of the article search is described in Figure 2.
Seroprevalence in this context refers to seropositivity with: (a) neutralizing antibodies to JEV (50% plaque reduction neutralization titers (PRNT50)) against JEV with a titer of ≥ 1:10; (b) anti-JEV serum IgM and IgG (enzyme-linked immunosorbent assay (ELISA)); or (c) micro virus neutralization > 1:20.4,10–12
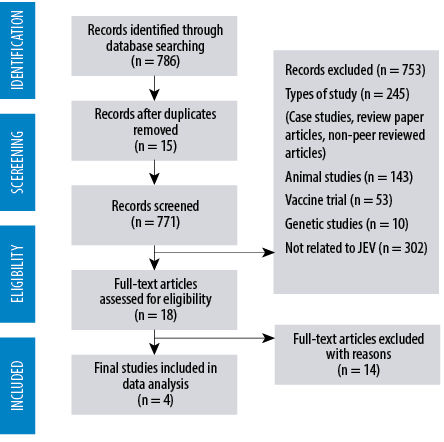
Figure 2: Results of literature search and evaluation of identified studies according to the PRISMA guidelines.
Table 1: Details of the included studies.
|
1 |
Hsu LC et al, 2014 |
Taiwan |
- |
Nationwide population |
6594 |
PRNT50 |
Not mentioned |
|
2 |
C Jeewandara et al, 2015 |
Sri Lanka |
Colombo |
Population attended a primary health care facility in the suburban areas of Colombo |
1689 |
ELISA |
Immune status ratio > 5 |
|
3 |
Lee EJ et al, 2016 |
South Korea |
Seoul |
Population in 10 provinces |
945 |
PRNT50 |
≥ 1:10 |
| |
|
|
Gyeonggi |
|
|
|
|
| |
|
|
Gangwon |
|
|
|
|
| |
|
|
Chungbuk |
|
|
|
|
| |
|
|
Chungnam |
|
|
|
|
| |
|
|
Jeonbuk |
|
|
|
|
| |
|
|
Jeonnam |
|
|
|
|
| |
|
|
Gyeongbuk |
|
|
|
|
| |
|
|
Gyeongnam |
|
|
|
|
| |
|
|
Jeju |
|
|
|
|
Table 2: Age-stratified seroprevalence of Japanese encephalitis virus according to survey years and vaccine introduction.
|
1 |
Taiwan |
2002 |
16–21 |
18.5 |
4 doses |
74 |
1968 |
| |
|
|
22–26 |
24 |
4 doses |
63 |
|
| |
|
|
27–32 |
29.5 |
3 doses |
55 |
|
| |
|
|
33–39 |
36 |
2 doses |
54 |
|
| |
|
|
40–49 |
44.5 |
- |
68 |
|
| |
|
|
50–90 |
70 |
- |
86 |
|
|
2 |
Sri Lanka |
2003 |
6–16 |
8.8a |
Mostly vaccinated; 1 or 4 doses |
28–44 |
1988
(Became national immunization program in 1988) |
| |
|
|
> 16 |
45a |
- |
> 44 |
| |
|
2014 |
6–16 |
8.8a |
Mostly vaccinated; 1 or 4 doses |
40–78 |
| |
|
|
> 16 |
45a |
- |
> 78 |
|
|
3 |
South Korea |
2010 |
30–39 |
34.5 |
1 dose |
97.8 |
1967
(Became mandatory in early 1980s) |
| |
|
|
40–49 |
44.5 |
May have been vaccinated |
97.9 |
|
| |
|
|
50–59 |
55.5 |
- |
98.3 |
|
| |
|
|
60–69 |
66.5 |
- |
98.3 |
|
|
4 |
India
Alapphuza |
2012 |
0–14 |
7 |
- |
15.6 |
2008 |
| |
|
|
15–44 |
29.5 |
- |
15.4 |
|
| |
|
|
45–64 |
54.5 |
- |
18.1 |
|
amean age for age cohort; *unable to determine.
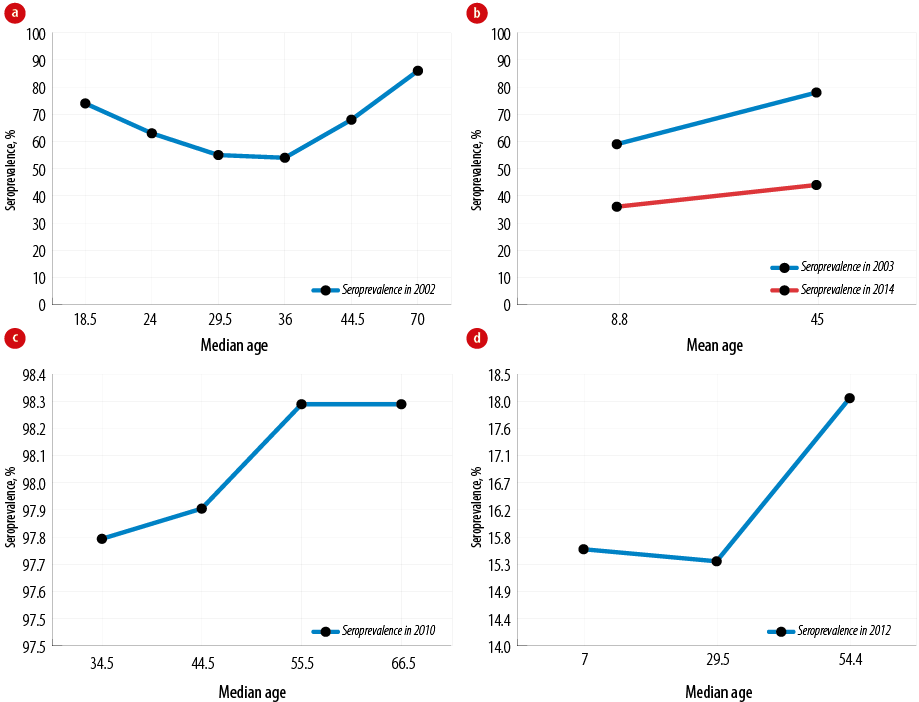
Figure 3: Age-stratified seroprevalence of Japanese encephalitis virus according to country and year.
All researchers independently extracted information from each article into an Excel sheet. The data was customized into: (a) code, (b) author and year of study publication, (c) country of study, (d) province or district of study, (e) population source, (f) sample size, (g) type of assay used, (h) assay threshold or dilution, (i) year of survey done, (j) age cohort, (k) median age, (l) JEV vaccination dose received, (m) seroprevalence, and (n) year of vaccine introduction. A second reviewer crossed-checked the articles assigned and provided comments in the table. Data were presented in tables and a graph to provide a visual summary of the changing seroprevalence by age over time. For standardization, the median age of each age cohort was determined for further analysis. In cases where the median could not be determined, but the mean value was available, the mean value was considered for graph tabulation.
Results
Four studies met the eligible criteria [Figure 2]. These studies were conducted in Taiwan, Sri Lanka, South Korea, and India and were coded according to the year of study publication [Table 1]. Study code 1 represented the whole country of Taiwan since data was collected from a nationwide population-based survey. Meanwhile, the other three studies (study codes 2, 3, and 4) presented data stratified by sub-geographic regions, with study code 3 consisting of 10 provinces in South Korea. The other two studies included only one district in the country.
Study references, countries and population sources, study assays, and their thresholds extracted from the selected studies are summarized in Table 1. Taiwan’s Centre for Disease Control conducted the first study in 2014.13 The following year, one study was conducted by the Centre of Dengue Research at a Sri Lankan tertiary education center.11 In 2016, the third study took place in South Korea by its Centre for Disease Control and Prevention, while the fourth study was conducted by the Indian National Institute of Virology in 2017.12,14
The timing and seasons of blood sample collection varied across all studies and took place from 2002 to 2014. The PRNT50 was used to determine seroprevalence in two studies (study codes 1 and 3), while the other two studies used ELISA IgG and micro virus neutralization assay, respectively, to profile neutralizing antibody responses (study codes 2 and 4). In the two studies that used the PRNT50 test, a titer of > 1:10 was considered seropositive. On the other hand, the study that used the micro virus neutralization assay considered cases positive if they had a dilution of > 1:20. In contrast, the study that used ELISA IgG considered cases of positive seroprevalence as those with an immune status ratio of more than five.
Table 2 summarizes the age-stratified sero-positivity rates obtained by the four studies by study year. Since the introduction of the JEV vaccination program in Taiwan in 1968, there have been multiple changes in the JEV doses given to its population ranging from two to three doses and finally, four doses according to birth cohorts. This study in 2002 showed that the eldest age group (50 to 90 years) had the highest seroprevalence rate of 86%, followed by the adolescent age group (16 to 21 years) with a seropositivity of 74%. The adult age group (33–39 years) had the lowest seroprevalence among all age groups at 54%.
Study code 2 conducted in Sri Lanka had lower JEV seroprevalence rates. In 2003, the children age group (6 to 15 years) had lower neutralized antibodies compared to the elder group (> 16 years), and this trend persisted until 2014, although the seroprevalence rates of both groups were seen to be higher in the latter year (28% vs. 44% in 2003 and 40% vs. 78% in 2014, respectively). Study code 3 conducted in South Korea showed a very high average seroprevalence rate (98.3%) among its adult and elderly populations. Among all age cohorts, those belonging to the 30–39 year group may have received one JEV vaccination dose, those aged 40–49 years might not have been vaccinated, while the rest of South Korea’s elderly cohort never had any JEV vaccination. The last study (code 4) represented an Indian population with relatively low JEV neutralized antibody rates compared to other Asian populations reviewed. In 2012, 45–64 years cohort scored the highest seropositivity (18.1%), followed by the 0 to 14 years (15.6%), 15 to 44 years (15.4%), and the > 65 years (12.9%) cohorts.
The trend for age-stratified seroprevalence was tabulated in a graph [Figure 3]. In general, there is an increasing trend of JEV seropositivity in all countries as their populations reach older ages. Nonetheless, there was a slight downtrend of seroprevalence among young adults in Taiwan and India before it increased again after the subjects reached a more mature age. It is also obvious that South Korea has the highest seroprevalence rate (97.8% to 98.3%) for all age cohorts compared to other countries, while India has the lowest seroprevalence rate (12.9% to 18.1%).
Discussion
The first JE case was recorded in 1891 in Japan. Since there are currently 24 endemic countries with the risk of JEV transmission identified. Twelve (50%) of the 24 countries had a JE immunization program in 2016; 10 (42%) programs were implemented nationally or subnationally in all risk areas, and two (8%) were subnational and did not include all risk areas.6,15
Of the four countries studied, Taiwan recorded the greatest number of age cohorts, enabling the authors to review its JEV age-stratified seroprevalence a little closer. The period of study survey in study code 1 began 34 years after the country initiated its mass vaccination program. The continuous rescheduling of the immunization policy has resulted in various birth cohorts receiving distinct doses of the JE vaccine. This study revealed that in 2002, the age-group-specific seroprevalence was the lowest among those 33 to 39 years old (54%) than among adolescents (74%) or the elderly (86%). These results might have been caused by the loss of antibodies because they either received the last dose long ago, received less than four doses of the vaccine, or received no vaccine at all. Conversely, a high seropositive rate of JEV neutralizing antibodies was found among people who were not vaccinated (i.e., the cohorts born before 1952). This is likely caused by a high frequency of early natural infection and accumulated exposure, which induces a stronger immunological memory response than that induced by vaccination.13,16
In study code 2, the differences between JEV seroprevalence and time can be seen since the study included two years of data in its survey (2003 and 2014) despite a lack of distinction of age stratification cohorts. It demonstrated that JEV seroprevalence of both median age groups had increased most likely due to the gap between the year the surveys were done with the year that the mass vaccine campaign was introduced in Sri Lanka, where they initially targeted higher-risk areas and later expanded the program in 1988.17
In contrast, the JEV seroprevalence was the highest in South Korea (study code 3), with an average of 98.3%. This is most likely because it was the earliest country to introduce the JEV vaccine in 1967, and vaccination was made mandatory in the early 1980s. Interestingly, old South Koreans who had no history of vaccination could also maintain a very high rate of JEV seropositivity (98.3%). Undoubtedly, this must be because of the natural infection that had led to this phenomenon.12 On the other hand, either vaccination or natural infection or both must have contributed to the very high seroprevalence rate among the rest of South Korea’s age cohorts.
WHO data for 2016 confirmed that all countries included in this review are covered for JE national vaccination with the exception of India, where the JEV vaccination program only covers high-risk and sentinel areas.6 Vaccination campaigns were introduced in 2008 in the studied district, a date much later than the other studied districts of the three other included countries, as shown in Table 2. Like other endemic districts in India, the live attenuated SA-14-14-2 vaccine against JEV was introduced as routine immunization under the Universal Immunization Program in 2011. Realizing that JE poses a great burden to their public health, the government of India announced the introduction of one dose of JE vaccine for adults in endemic districts in its national vaccination program in 2014.18 Hence, the age cohorts included in this study had never received any JEV vaccination. This probably explains why study code 4’s population has the lowest JEV seroprevalence among all.
Several serological methods were used in studying antibody responses to JE, including neutralization, hemagglutination inhibition (HI), CFT, ELISA, and the indirect fluorescent antibody test (IFA). However, antibodies measured by HI, CFT, ELISA, and IFA do not correlate with protection. Only neutralizing antibodies correlate with protection. The neutralization test is the most specific measure of antibody (i.e., it has little cross-reaction with other flaviviruses). To measure neutralizing antibody titers, the PRNT50 is most often used. The essence of the test is that when JEV is grown on a cell monolayer, it causes plaques to form. The number of plaques formed is reduced if the virus has been mixed with serum containing neutralizing antibodies, and this reduction in plaques measures the antibody titer (WHO1). Most studies recommend an end-point of 50% reduction in PRNT50, but no international standard for the exact procedure or choice of end-points has been established.10
There are a few limitations noted in this study. All blood samples taken for seroprevalence analysis were collected in a 12-year range (2002 to 2014) with inconsistencies in the definition of age cohorts in each study. The dosage and type of JEV vaccination given were also not the same either inter- or intra-nationally. All these resulted in difficulty in producing a standard comparison. Finally, the assays used for JEV neutralizing antibody detection were also not standardized in this review. PRNT50 is the most reliable method for detecting vaccine-induced JEV antibodies, while ELISA is more suitable for diagnosis because the chance of confusion with vaccine-induced antibodies is relatively low.19
Despite these limitations, findings in this study indicate that JEV seroprevalence increases with age, and its high seropositivity rate can be maintained with thorough implementation of national or universal vaccination programs. More specifically, this study also indicated that protective immunity remains high in adults who received vaccinations during childhood up until at least 30 years before natural immunity becomes superior in the older population. The data compiled highlighted consistent changes in age-stratified JEV seroprevalence; hence, proving that increasing age does increase a person’s susceptibility to the disease. In other words, it may aid in the identification of vulnerable populations. Although there is contradicting evidence on higher seroprevalence among vaccine-naïve populations, vaccination remains highly recommended until today. Such a situation is supported by many studies; a study in Japan reported that naïve populations with detectable neutralizing antibodies had higher annual infection rates compared to populations with vaccination histories. This signifies that in Japan, JEV remains present and active in nature; thus, continuing the JEV vaccination program is indispensable to prevent JE infection in humans.20
Conclusion
Although JE remains a prominent public health concern in the Western Pacific region, reported cases have decreased mainly due to JE immunization. However, as JEV will remain in nature and the zoonotic chains, the risk of infection will persist. Hence, it is important to apply JEV vaccination protocols in national immunization programs, prioritizing young children.
Disclosure
The authors declared no conflicts of interest. No funding was received for this study.
references
- 1. Simon LV, Sandhu DS, Goyal A, Kruse B. Japanese encephalitis. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2020.
- 2. Zheng Y, Li M, Wang H, Liang G. Japanese encephalitis and Japanese encephalitis virus in mainland China. Rev Med Virol 2012 Sep;22(5):301-322.
- 3. World Health Organization. The immunological basis for immunization series module 13: Japanese encephalitis. Immunization, vaccines and biologicals. Geneva: World Health Organization; 2010.
- 4. World Health Organization. Japanese encephalitis. Geneva. 2019 [cited 2019 May 9]. Available from: https://www.who.int/news-room/fact-sheets/detail/japanese-encephalitis.
- 5. Campbell GL, Hills SL, Fischer M, Jacobson JA, Hoke CH, Hombach JM, et al. Estimated global incidence of Japanese encephalitis: a systematic review. Bull World Health Organ 2011 Oct;89(10):766-774, 774A-774E.
- 6. Heffelfinger JD, Li X, Batmunkh N, Grabovac V, Diorditsa S, Liyanage JB, et al. Japanese encephalitis surveillance and immunization—Asia and Western Pacific Regions, 2016. MMWR Morb Mortal Wkly Rep 2017 Jun;66(22):579-583.
- 7. Fischer M, Hills S, Lindsey N, Staples JE. Japanese encephalitis vaccines; recommendations of the advisory committee on immunization practices (ACIP); 2010.
- 8. Pan JR, Yan JY, Zhou JY, Tang XW, He HQ, Xie RH, et al. Sero-molecular epidemiology of Japanese encephalitis in Zhejiang, an eastern province of China. PLoS Negl Trop Dis 2016 Aug;10(8):e0004936.
- 9. Choe YJ, Taurel AF, Nealon J, Seo HS, Kim HS. Systematic review of seroepidemiological studies on Japanese encephalitis in the Republic of Korea. Int J Infect Dis 2018 Feb;67:14-19.
- 10. Timiryasova TM, Bonaparte MI, Luo P, Zedar R, Hu BT, Hildreth SW. Optimization and validation of a plaque reduction neutralization test for the detection of neutralizing antibodies to four serotypes of dengue virus used in support of dengue vaccine development. Am J Trop Med Hyg 2013 May;88(5):962-970.
- 11. Jeewandara C, Gomes L, Paranavitane SA, Tantirimudalige M, Panapitiya SS, Jayewardene A, et al. Change in dengue and Japanese encephalitis seroprevalence rates in Sri Lanka. PLoS One 2015 Dec;10(12):e0144799.
- 12. Balakrishnan A, Thekkekare RJ, Sapkal G, Tandale BV. Seroprevalence of Japanese encephalitis virus & West Nile virus in Alappuzha district, Kerala. Indian J Med Res 2017 Jul;146(Supplement):S70-S75.
- 13. Hsu LC, Chen YJ, Hsu FK, Huang JH, Chang CM, Chou P, et al. The incidence of Japanese encephalitis in Taiwan–a population-based study. PLoS Negl Trop Dis 2014 Jul;8(7):e3030.
- 14. Lee EJ, Cha GW, Ju YR, Han MG, Lee WJ, Jeong YE. Prevalence of neutralizing antibodies to Japanese encephalitis virus among high-risk age groups in South Korea, 2010. PLoS One 2016 Jan;11(1):e0147841.
- 15. Erlanger TE, Weiss S, Keiser J, Utzinger J, Wiedenmayer K. Past, present, and future of Japanese encephalitis. Emerg Infect Dis 2009 Jan;15(1):1-7.
- 16. Hills SL, Weber IB, Fischer M. Japanese encephalitis. In: Centers for disease control and prevention. CDC health information for international travel 2014. New York: Oxford University Press; 2014.
- 17. Baig S, Fox KK, Jee Y, O’Connor P, Hombach J, Wang SA, et al; Centers for Disease Control and Prevention (CDC). Japanese encephalitis surveillance and immunization–Asia and the Western Pacific, 2012. MMWR Morb Mortal Wkly Rep 2013 Aug;62(33):658-662.
- 18. Vashishtha VM, Ramachandran VG. Vaccination policy for Japanese encephalitis in India: tread with caution! Indian Pediatr 2015 Oct;52(10):837-839.
- 19. Cha GW, Cho JE, Ju YR, Hong Y-J, Han MG, Lee W-J, et al. Comparison of four serological tests for detecting antibodies to Japanese encephalitis virus after vaccination in children. Osong Public Health Res Perspect 2014 Oct;5(5):286-291.
- 20. Konishi E, Kitai Y, Tabei Y, Nishimura K, Harada S. Natural Japanese encephalitis virus infection among humans in west and east Japan shows the need to continue a vaccination program. Vaccine 2010 Mar;28(14):2664-2670.