An 81-year-old man with multiple comorbidities presented with a two-year history of dysphonia. The patient had visited multiple clinics to no avail. He also reported occasional foreign body sensation, which was not bothersome. Besides that, there were no constitutional symptoms, regurgitation, or halitosis. No cough, dysphagia, or neck swelling were mentioned. Examination revealed a hoarse voice with no audible stridor. His vital signs, as well as baseline blood investigations, were within normal parameters. Oral cavity and neck examinations were unremarkable. Valsalva maneuver demonstrated no neck swelling. Flexible nasopharyngolaryngoscopy performed showed mild subcordal edema with no suspicious lesion. Barium swallow demonstrated bilateral outpouching of the hypopharynx, which was larger on the left [Figure 1].
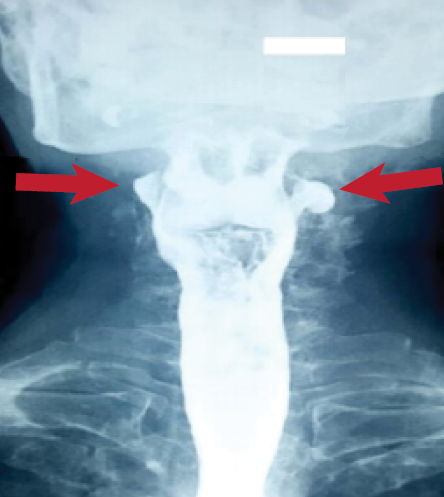
Figure 1: Barium swallow showing bilateral outpouching of the hypopharynx.
Question
What is the most likely diagnosis?
a) Laryngocele.
b) Saccular cyst.
c) Laryngeal malignancy.
d) Pharyngeal pouch.
Answer
d) Pharyngeal pouch.
Treatment options were discussed with the patient, along with the complications. The patient opted for conservative management, weighing the devastating complications. The patient is currently followed-up regularly with no worsening symptoms.
Discussion
Pharyngeal pouch (PP), a pseudodiverticulum, is a protrusion of pharyngeal mucosa through Killian’s dehiscence (a weak area in the posterior wall of the pharynx). Albeit unknown, recent etiology is associated with improper relaxation of cricopharyngeal muscle upon swallowing.1 Classical presentation of PP includes dysphagia, regurgitation of undigested food, chronic cough, halitosis, and weight loss. Hoarseness has been reported rarely.2 Symptoms become commensurate with the growing PP.3 Additionally, rapid progression or severity of the symptoms suggests malignancy.4 PP can either be posterior, posterolateral, or lateral, with posterior being the most common type.3 The presence of aperture at Killian’s dehiscence has been advocated as the attribute, albeit dual PP has been described.5 It is interesting to note that the laterality of the entity is related to the handedness of the patient, despite the left side being the most common.6
Barium swallow is considered sine qua non in diagnosing PP and has been reckoned as the gold standard as it outlines the pouch. Clinical findings are scarce upon presentation. Boyce sign—neck swelling which gurgles upon palpation—is often regarded as a proxy of this entity. Surgery is the primary mode of treatment, either via external or endoscopic approach. Each surgery carries daunting risks and complications that should be borne in mind, as patients with PP are generally elderly with multiple comorbidities. Close observation ought to be exercised, weighing the significant mortality and morbidity that accompanies
this entity.2
Disclosure
The patient gave consent to publish the image.
references
- Peters JH, Mason R. [The physiopathological basis for Zenker’s diverticulum]. Chirurg 1999 Jul;70(7):741-746.
- 2. Siddiq MA, Sood S, Strachan D. Pharyngeal pouch (Zenker’s diverticulum). Postgrad Med J 2001 Aug;77(910):506-511.
- 3. Bowdler DA. Pharyngeal pouches. In: Kerr A, ed. Scott Brown’s textbook of otorhinolaryngology. 6th ed. Oxford: Butterworth-Heinmann; 1997. p. 1-21.
- 4. Bradley PJ, Kochaar A, Quraishi MS. Pharyngeal pouch carcinoma: real or imaginary risks? Ann Otol Rhinol Laryngol 1999 Nov;108(11 Pt 1):1027-1032.
- 5. Meehan T, Henein RR. An unusual pharyngeal pouch. J Laryngol Otol 1992 Nov;106(11):1002-1003.
- 6. Stafford ND, Moore-Gillon V, McKelvie P; StaVord ND. Handedness and the side on which pharyngeal pouches occur. Br Med J (Clin Res Ed) 1984 Mar;288(6420):815-816.