A 46-year-old woman presented with a huge, hard sternal mass with a one -year history. The size of the mass has been progressively increasing from an initial size of a table tennis ball. It was dull and aching in nature with a sensation of heaviness, which affected her daily life activities and made her seek medical attention. The mass was associated with skin discoloration and contact bleeding. There was no fever. Clinically, despite being hard and fixed, it tended to pulsate with bruit on auscultation [Figure 1]. She had a total thyroidectomy for a multinodular goiter 10 years prior, but defaulted follow-up soon after the surgery. She was on thyroid replacement therapy, but decided to stop taking it for the past two years due to a logistic issue.
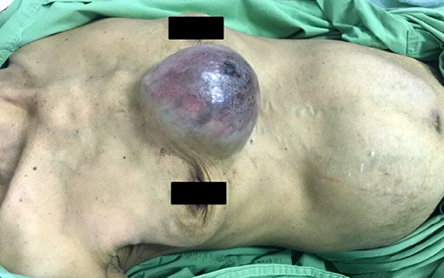
Figure 1: Huge anterior chest mass with discoloration and pulsatile in character.
Question
- What is the most likely clinical diagnosis?
a. Ewing sarcoma.
b. Osteosarcoma.
c. Osteoblastoma.
d. Multiple myeloma.
e. Metastatic follicular thyroid carcinoma.
Answer
e. Metastatic follicular thyroid carcinoma.
Discussion
Our patient had a metastatic lesion of follicular thyroid carcinoma. Metastasis commonly occurs via hematogenous spread. It uncommonly presents with a mass of a flat bone, namely skull and sternum. Follicular thyroid cancer is the second most common well-differentiated thyroid malignancy after papillary thyroid carcinoma. Pulsatile mass is the pathognomonic sign of metastasis from follicular thyroid malignancy. Usually, late presentation is rare, but it can appear after 10 years post-total thyroidectomy, as in our case, and even up to 13 years later.1 Hence, it gives a diagnostic dilemma of either primary sternal lesion or secondary metastasis from the thyroid.1 The role of biopsy is undeniably paramount to distinguish between those two pathologies.
Ewing sarcoma tends to develop in children and young adults. It mostly affects long bones such as femur, tibia, and humerus. Pain on the involved site is the most common complaint experienced by the patients. Osteosarcoma or osteogenic sarcoma is the most common bone cancer among children. Similar to Ewing sarcoma, it also arises from the long bones, but it unfolds from the bone end where the cells are actively dividing, such as proximal tibia, distal fibula, and proximal humerus. Osteoblastoma is considered as a disease of youngsters. It is a slow-growing benign bone tumor that rarely turn malignant. It is located in long bone but mostly arises at the spine causing bone pain. Multiple myeloma can manifest as bone pain, symptoms of pancytopenia, spinal cord compression, and features of renal failure. It is rare to find multiple myeloma presenting with a huge bony mass.
Surgery is the mainstay of treatment in managing secondary metastasis of follicular thyroid cancer, not only to ensure the effectiveness of radioactive iodine therapy but also to improve the cosmetic result and quality of life. Occasionally, the sternal mass can be complicated with infiltrations to the airway or esophagus and compression to the lung, causing asphyxia. The sternal metastasis can be resected following oncologic intention by doing sternectomy, rib resection if required, sternoplasty with titanium mesh and acrylic plate for closure of sternal defect.2 Polypropylene mesh reconstruction even can be chosen as an alternative. However, those techniques are futile and trivial in a hostile environment intraoperatively, especially in infected tissue or R2 resection. In such situations, closure of the defect can be obtained by performing a myocutaneous free flap or bilateral pectoralis major flap reconstruction.3
In conclusion, in managing advanced sternal metastasis, palliative resection with reconstruction of the defect is mandatory for subsequent radioactive iodine therapy and thyroid suppressive treatment. Hence, they can improve the patient’s quality of life afterward.
references
- 1. Eroglu A, Karaoglanoglu N, Bilen H, Gursan N. Follicular thyroid carcinoma: metastasis to the sternum, 13 years after total thyroidectomy. Int J Clin Pract 2006 Nov;60(11):1506-1508.
- 2. Syazni MA, Gendeh HS, Kosai NR, Ramzisham AR, Gendeh BS, Basiron NH, et al. Follicular thyroid cancer with sternal metastasis - challenges and outcomes. Med J Malaysia 2017 Feb;72(1):80-82.
- 3. Adwin Z, Nur A, Suhaimi S, Rahman R. Surgical management of bulky mediastinal metastases in follicular thyroid carcinoma. Oman Med J 2016 Jan;31(1):69-72.